Brentwood: (615) 235-1966

Tooth Decay Process: Ways to Stop It Before a Cavity Forms
Brentwood and Lewisburg, TN
A cavity doesn’t happen overnight. There’s a whole process that unfolds before a tooth needs a filling, and for a meaningful stretch of that process, the damage is actually reversible. That window doesn’t stay open forever, but it exists, and knowing how to use it changes what’s possible for your long-term dental health.
How Tooth Decay Develops
Decay is the result of a biological cycle playing out repeatedly in your mouth. Bacteria like Streptococcus mutans feed on the sugars and refined carbohydrates in your diet and produce acids as a byproduct. Those acids lower the pH in your mouth and begin to pull minerals from your tooth enamel, a process called demineralization. Your saliva works to reverse this by redepositing minerals and buffering acid, but when demineralization outpaces remineralization, enamel starts to weaken.
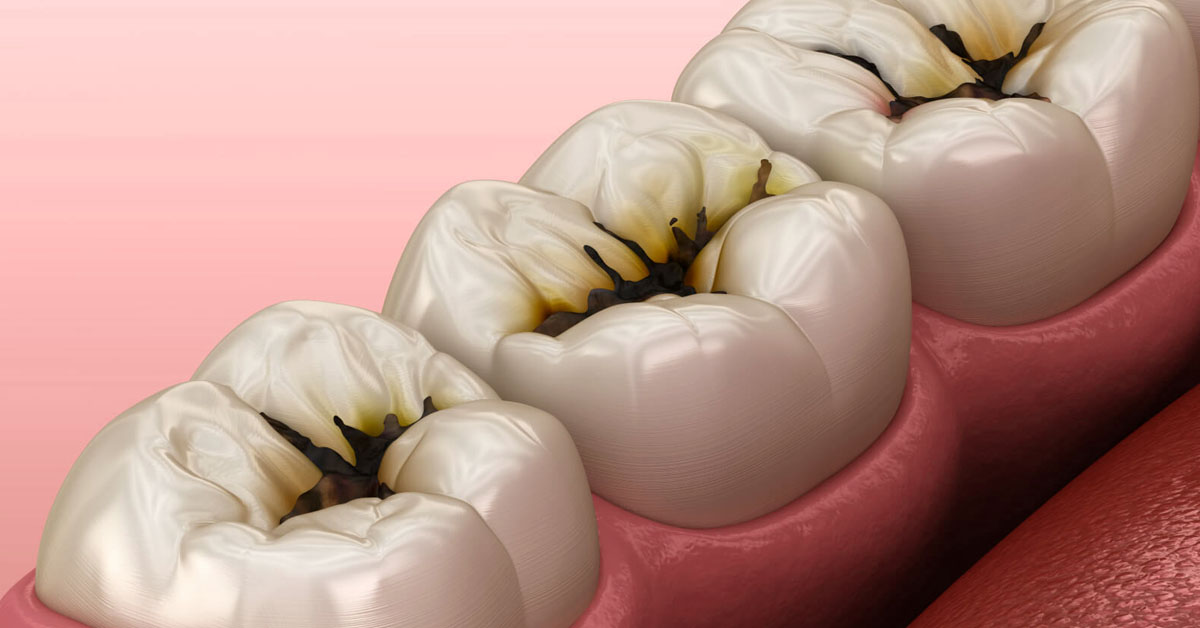
This early stage of mineral loss may appear as a faint white spot on the tooth surface, the only visible sign. But left unaddressed, it progresses. The enamel softens, then breaks down, and eventually a cavity forms. At that point, the decay can no longer be reversed and needs to be removed and replaced with a filling.
One of the most effective ways to interrupt this cycle before it reaches that point is through protective treatments like dental sealants. At Hallmark Dental, patients who come in for routine care are often surprised to learn how much can be done to stop decay before it ever requires a drill.
The Five Stages of Tooth Decay
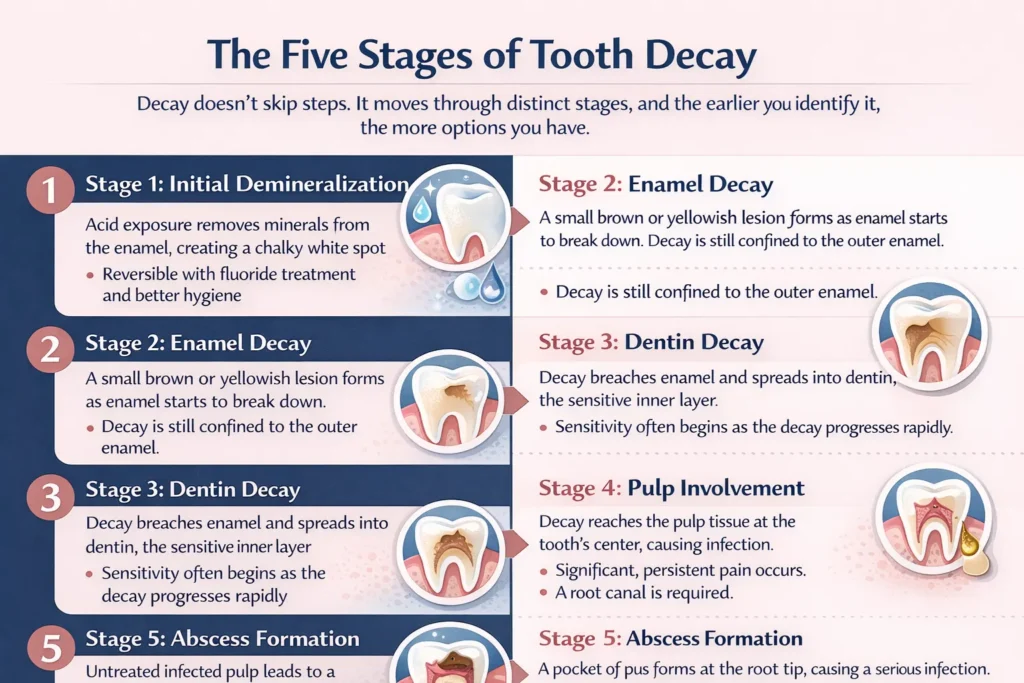
Decay doesn’t skip steps. It moves through distinct stages, and the earlier you identify it, the more options you have.
Stage 1: Initial Demineralization
Acid exposure has begun pulling minerals from the outer enamel. A faint white or chalky spot may appear on the tooth surface. This stage is fully reversible with fluoride treatment and improved hygiene habits.
Stage 2: Enamel Decay
The enamel has weakened enough to develop a small lesion. The surface may appear brown or yellowish. At this point, the decay is still confined to enamel and hasn’t reached the deeper layers of the tooth.
Stage 3: Dentin Decay
Once decay breaches the enamel and reaches the dentin (the softer layer beneath), it progresses rapidly. Dentin is less resistant to acid and contains microscopic tubules that connect to the tooth’s nerve, which is why sensitivity often begins at this stage.
Stage 4: Pulp Involvement
The decay has reached the pulp, the soft tissue at the center of the tooth that houses nerves and blood vessels. Pain becomes more significant and consistent. A root canal is typically required at this stage.
Stage 5: Abscess Formation
An untreated infected pulp can lead to a dental abscess – a pocket of pus at the root tip. This is a serious condition that requires immediate treatment and, in some cases, can affect surrounding bone and tissue.
The first two stages are where intervention is simplest. Stages three through five involve progressively more invasive and costly treatment. Getting ahead of decay early isn’t just better for your health – it’s better for your wallet and your time.
What Stops Decay Before a Cavity Forms
Fluoride: Your Enamel’s First Line of Defense
Fluoride is the most well-studied cavity prevention tool available. It strengthens enamel by incorporating into the tooth structure and making it more resistant to acid attack. It also facilitates remineralization – the process of restoring minerals to weakened enamel. Fluoride toothpaste used twice daily is the foundation of any sound prevention strategy. For patients at higher risk, prescription-strength fluoride, fluoride varnish applied at dental visits, or fluoride rinses can provide additional protection.
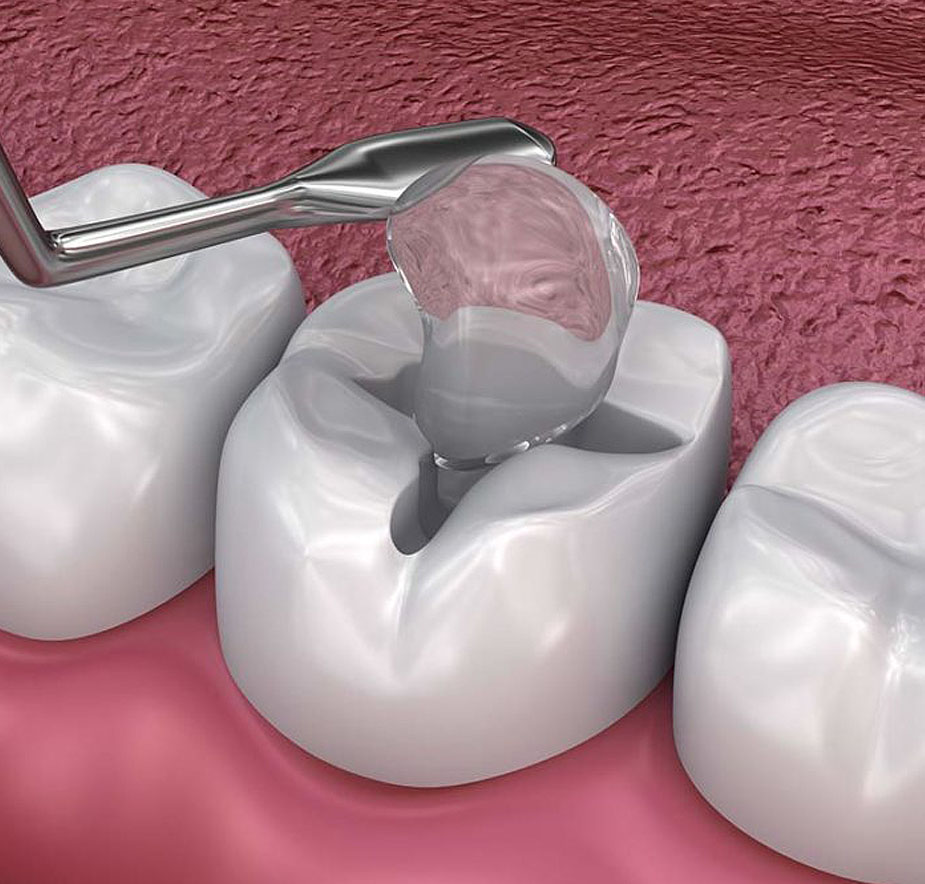
Dental Sealants: Physically Blocking Decay
The chewing surfaces of back teeth (molars and premolars) are covered in deep grooves and pits where food debris and bacteria collect easily. These areas are notoriously difficult to clean with a toothbrush and account for a disproportionate share of cavities, particularly in children and teenagers.
Dental sealants are thin, protective coatings made of a resin or glass ionomer material that are applied to grooved surfaces and hardened in place. They physically seal out bacteria and food, preventing the conditions that lead to decay. According to the Centers for Disease Control and Prevention (CDC), sealants prevent about 80% of cavities in the back teeth during the first two years after application and continue to protect against 50% of cavities for up to four years. They’re among the most cost-effective preventive treatments in dentistry.
Consistent Oral Hygiene
Brushing twice daily with a fluoride toothpaste, flossing once daily, and limiting between-meal snacking reduce the frequency of acid attacks on your enamel. Every time you eat fermentable carbohydrates, your mouth becomes acidic for roughly 20 to 30 minutes. If you’re snacking constantly throughout the day, your enamel never gets a real recovery window. Three structured meals with water in between give saliva time to do its job.
Diet Modifications That Matter
Cutting back on sugary and acidic beverages like sodas, sports drinks, and fruit juices reduces the fuel available to decay-causing bacteria. Drinking water throughout the day, particularly fluoridated tap water, supports both hydration and remineralization. Cheese, nuts, and leafy greens provide calcium and phosphate, the minerals that make up your enamel.
Regular Professional Cleanings and Exams
Your dentist and hygienist can detect early-stage demineralization that you’d never notice on your own. They can remove tartar from surfaces that brushing misses, apply fluoride varnish, and monitor areas that look vulnerable before they become actual cavities. Biannual visits are the standard recommendation for most patients, though those at higher risk of decay may benefit from more frequent cleanings.
Put It Together
The decay process is consistent and predictable, so your prevention strategy can be, too. Fluoride remineralizes weakened enamel, dental sealants block the grooves most vulnerable to bacterial buildup, good hygiene disrupts the plaque that drives acid production, and regular dental visits catch problems when they’re still manageable.
Hallmark Dental works with patients to build prevention plans that fit their actual risk level, not a generic checklist. Whether you’re bringing in a child for their first sealants or addressing early signs of enamel wear in your own teeth, the approach is the same: find what’s happening early, and deal with it before it requires more.
Book your appointment at Hallmark Dental today.
People Also Ask
The American Dental Association recommends sealants as soon as the first permanent molars come in, typically around age 6, and again when the second permanent molars appear around age 12. That said, teens and adults with deep grooves and no existing decay in those teeth can also benefit. Age matters less than whether the tooth is vulnerable and decay-free at the time of application.
Sealants last between five and ten years, though this varies depending on chewing habits and the specific material used. They’re checked at every routine dental visit and can be reapplied if they chip, wear down, or partially detach. Even a partially intact sealant still offers some protection.
Early-stage decay before an actual cavity forms can be reversed through remineralization. This requires consistent fluoride exposure, reduced sugar intake, and good saliva flow. Once decay has progressed through the enamel into dentin, reversal is no longer possible, and restoration is required.
Yes, with caveats. Sugar-free gum sweetened with xylitol stimulates saliva flow, which helps neutralize acids and remineralize enamel. Xylitol itself also inhibits the growth of Streptococcus mutans. Chewing it for 20 minutes after meals is a reasonable supplementary habit, though it doesn’t replace brushing or flossing.
Not always. White spots can also result from fluorosis (excess fluoride during tooth development), enamel hypoplasia, or demineralization from orthodontic brackets. A dentist can distinguish between these causes during an exam. When a white spot is confirmed as early demineralization, it can often be treated non-invasively with remineralizing agents before a cavity develops.