Brentwood: (615) 235-1966

Dental Implants for Smokers: What You Should Know
Brentwood and Lewisburg, TN
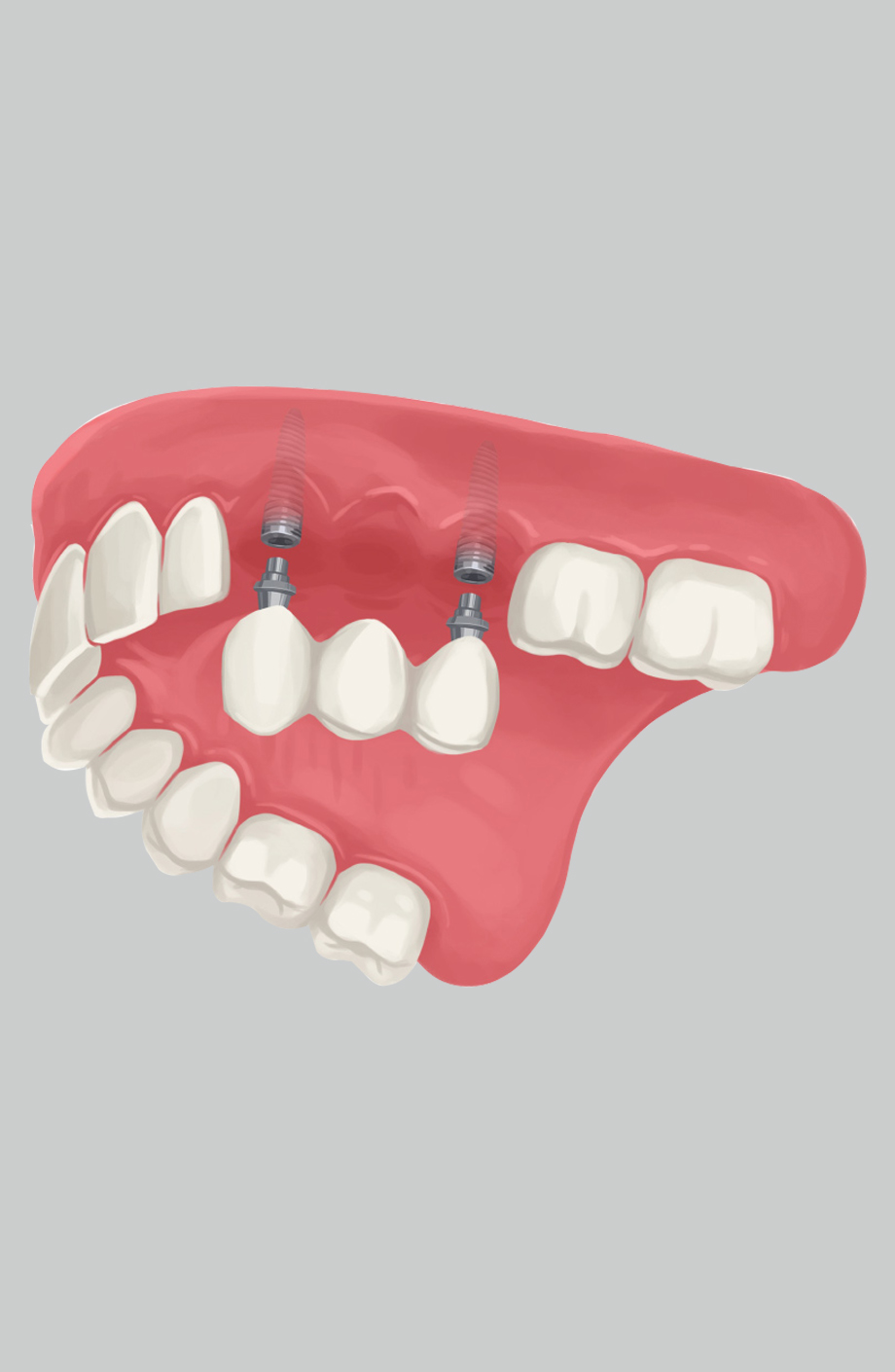
Smoking and dental implants are a combination that comes up often in consultations, and for good reason. Patients who smoke want honest answers, not a flat-out refusal or a vague warning that leaves them more confused than when they started. The reality is nuanced. Smoking does not automatically disqualify you from getting implants, but it does meaningfully change the risk profile of the procedure and the steps needed to give your implant the best chance of lasting.
Here is what the research actually says, what you need to know before your consultation, and what you can do to improve your outcome.
How Smoking Affects Implant Success
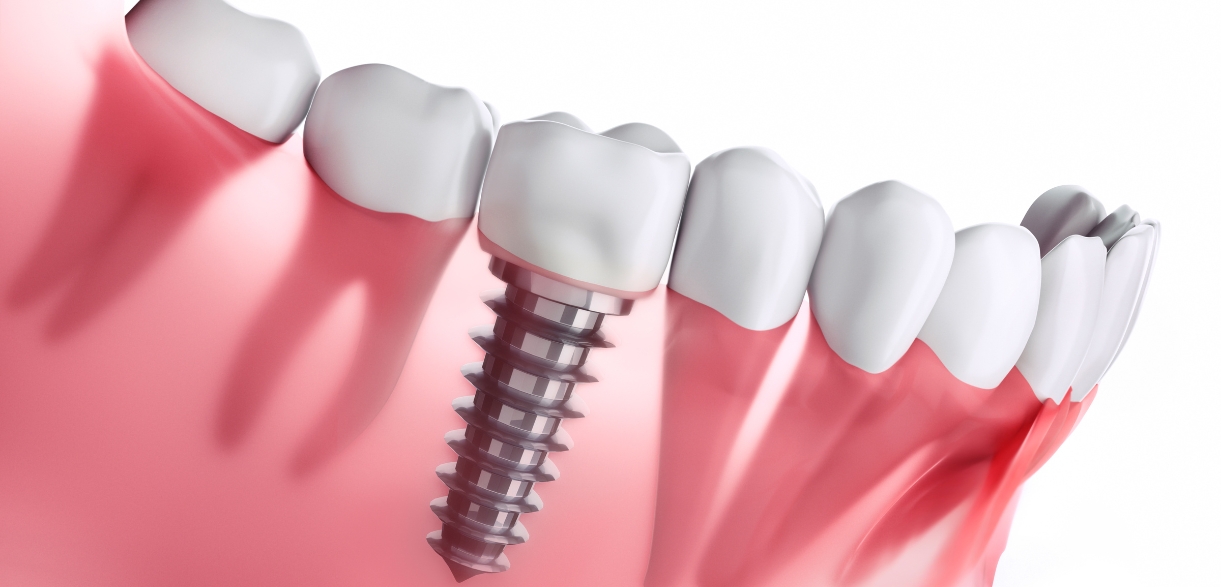
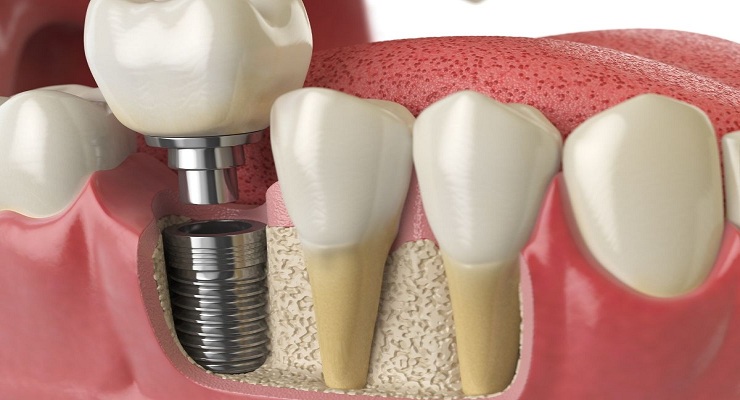
Dental implants work by osseointegration, the biological process in which the titanium post fuses with the surrounding jawbone over several months. This process depends heavily on healthy blood flow, adequate immune response, and undisturbed healing of the surrounding soft tissue.
Smoking disrupts all three. Nicotine constricts blood vessels, which reduces circulation to the gum tissue and bone around the implant site. Carbon monoxide from cigarette smoke displaces oxygen in the bloodstream, further limiting the nutrients available to healing tissue. At the same time, the chemicals in tobacco suppress immune function, slowing the body’s response to infection and tissue repair.
Dental implants in Lewisburg follow the same biological principles as implants placed elsewhere, which means these systemic effects are just as relevant for patients in Middle Tennessee as they are anywhere in the country.
A 2012 study published in the Journal of Dental Research found that smokers had a significantly higher rate of implant failure compared to non-smokers, with the risk particularly elevated in the early healing phase and for implants placed in the upper jaw. More recent research continues to support this finding, with failure rates in smokers estimated to be roughly twice that of non-smokers in some studies.
That said, many smokers do receive dental implants and have them succeed long-term. The key lies in preparation, timing, and commitment to the process.
The Risks Smokers Face
Understanding the particular complications that smoking introduces helps frame the conversation with your dentist honestly.
Peri-implantitis
This is the implant equivalent of gum disease. It involves inflammation and infection of the tissue and bone surrounding the implant and can lead to bone loss and, eventually, implant failure if left untreated. Smokers are at a substantially elevated risk of developing peri-implantitis because of the immune-suppressing and circulation-reducing effects of tobacco. The condition can develop years after a successful placement, which is why long-term maintenance matters just as much as the initial healing phase.
Delayed Healing and Dry Socket Risk
Following implant surgery, the surgical site needs time to close and stabilize. Smoking slows this process. The suction involved in smoking can also disturb the clot that forms over the extraction site if a tooth is removed in preparation for the implant, increasing the risk of dry socket, a painful condition that delays healing further.
Bone Loss Around the Implant
Smoking is a known risk factor for alveolar bone loss, which affects the density and volume of the jaw. For implants to remain stable over time, the surrounding bone needs to maintain its structure. Patients who smoke over the long term may experience more gradual bone loss around the implant post, which can compromise stability years down the line.
Soft Tissue Complications
Gum tissue around an implant needs to form a healthy seal to protect the implant from bacteria. Smoking impairs soft tissue’s ability to heal and attach properly, leaving the implant site more vulnerable to bacterial infiltration, particularly in the months immediately following placement.
What You Can Do to Improve Your Odds
None of this means implants are off the table. It does mean that going in without any preparation unnecessarily increases the likelihood of complications. There are concrete steps that make a real difference.
Stop Smoking Before and After Surgery
The most impactful thing a smoker can do is quit, at least temporarily, around the time of surgery. Most dental providers recommend stopping smoking at least one week before the procedure and for a minimum of two months after, covering the critical osseointegration period. Some research suggests that patients who quit smoking even temporarily for surgery have outcomes closer to non-smokers than to active smokers who continue throughout the healing phase.
Permanently quitting, of course, is better for your implant and your overall health. Tennessee has several free cessation resources available, including the Tennessee Tobacco QuitLine (1-800-QUIT-NOW), which provides coaching and support at no cost to residents.
Maintain Rigorous Oral Hygiene
This matters for every implant patient, but it is especially critical for smokers. Brushing twice daily, flossing carefully around the implant site, and using an antimicrobial rinse as directed reduce the bacterial load in the mouth and help offset some of the immunosuppressive effects of tobacco. Your dentist Lewisburg in may recommend a tailored oral home care protocol for your dental condition.
Keep Every Follow-Up Appointment
The monitoring phase after implant placement is where complications are caught early. For smokers, regular professional cleanings and implant check-ups are not optional extras. They are the mechanism by which peri-implantitis and bone changes are detected before they reach a point of no return. Missing appointments increases the risk considerably.
Be Transparent With Your Dental Specialist
Your dental provider needs an accurate picture of your smoking history, current frequency, and any other health factors to plan the right approach. That includes whether you use smokeless tobacco or vaping products, both of which carry overlapping risks with traditional cigarettes. The more complete the information, the more tailored and realistic your treatment plan can be.
Patients who come in prepared, with a realistic picture of the risks and a willingness to follow the pre- and post-surgical protocols, tend to do considerably better than those who do not. That holds true whether you are a light occasional smoker or someone who has smoked heavily for years.
Smoking raises implant failure risk. That is a fact supported by consistent research. But it does not make implants impossible, nor does it mean you have to give up on replacing missing teeth with a permanent, functional solution.
This means the process requires more planning, higher commitment to aftercare, and a frank conversation with your dental provider about realistic expectations. Patients who go in with clear eyes and follow the guidance they are given tend to achieve outcomes they are genuinely happy with.
If you are in the Lewisburg area and want to find out whether you are a candidate, call Hallmark Dental’s office to schedule a consultation. Bring your questions. The conversation is more straightforward than you might expect.
People Also Ask
Long-term smoking history does not automatically disqualify you from implants, but it does require a thorough evaluation of your bone density and gum health, both of which can be affected over time. Your dentist will assess whether you have sufficient bone volume for implant placement and whether any preparatory procedures, such as bone grafting, are needed before moving forward.
Research on vaping and implant outcomes is still emerging, but current evidence suggests that the nicotine in e-cigarettes produces similar vasoconstrictive and healing-related effects as traditional cigarettes. Patients who vape should disclose this to their dentist before implant surgery, as the risks are not negligible simply because the delivery method differs from combustible tobacco.
Most providers recommend stopping at least one week before surgery, though longer is better. The two months following surgery are considered the most critical healing period, and abstaining from smoking throughout this window substantially reduces failure risk. Some providers will ask patients to demonstrate a smoking cessation plan before proceeding.
Insurance coverage for dental implants varies widely by plan and is unrelated to smoking status in most cases. Most dental plans cover little to no part of the implant cost, though financing options are often available. Your dental office can help you review your benefits and discuss payment plan options before committing to treatment.
Implant failure most often presents as persistent pain, mobility of the implant post, or infection at the surgical site. If failure occurs, the implant is typically removed, the site is allowed to heal, and the possibility of replacement is evaluated once healing is complete. In some cases, bone grafting is needed before a second implant attempt. Success rates for replacement implants are generally reasonable, if the underlying risk factors, including smoking, have been addressed.